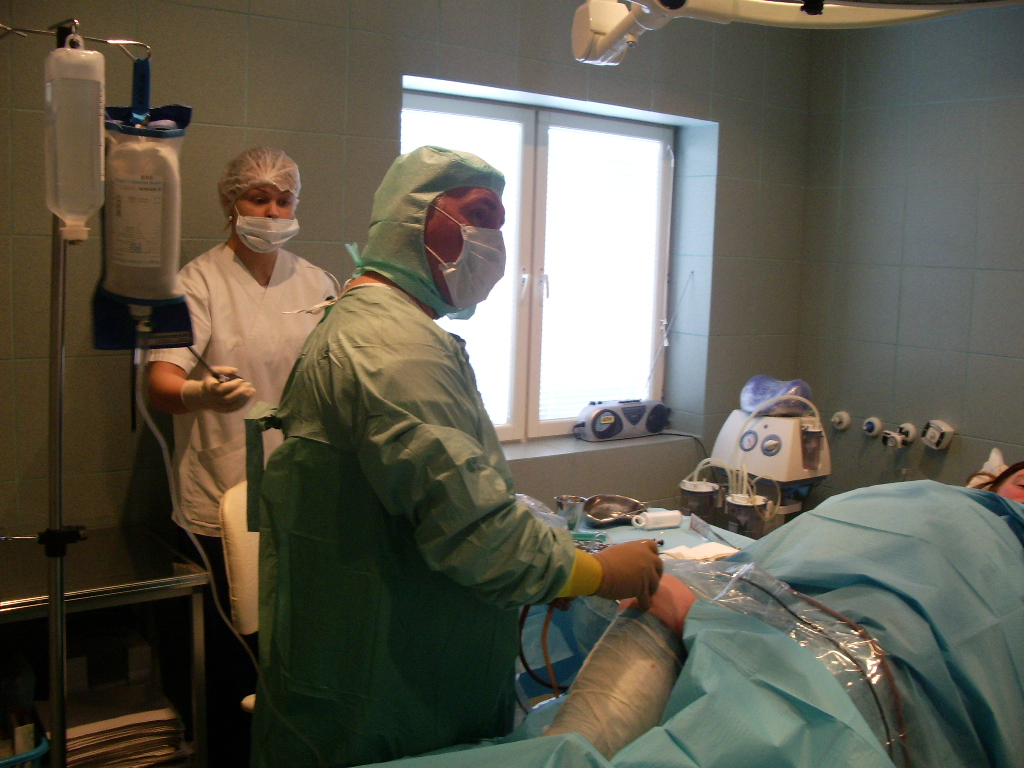
In our private clinic we made about 400 different general surgical operations in one year.
- varicosity
- hemorrhoids
- hernias
- ganglions cysts
Varicose – Enlarged leg veins – Leg varicosity
Method of atraumatic stripping in removing enlarged leg veins. The main advantages of atraumatic stripping compared to standard methods are a significantly shorter recovery period and sick leave. Varicose or enlarged veins are a problem that occurs to a lot of people. It is manifested by a swelling in the ankle area, an enlargement of superficial veins, which are usually the first symptoms of this disease, a feeling of heaviness and numb pains in the shin. Besides the already listed symptoms, patients that suffer from these problems complain about tingles and itching in the legs. If the problem of enlarged veins is neglected, it may come to complications such as ruptures and bleeding from the enlarged vein, an inflammation of the superficial veins (tromboflebitis), chronic vein insufficiency characterized by swelling of the shin, inner ankle callosity, hyperpigmentation and, in the end, an open wound which is usually very resistant to treatment! The most important natural factors in developing varicosity are weakly developed or undeveloped vein valves of the superficial veins (this is where the heredity factor plays the most important role), lack of physical activity, long sitting and/ or standing, prior leg injuries. However, it is important to point out that the function reduction (insufficiency) of valves has the most important role in developing varicosity. Because of the insufficiency of the so called safeno-femoral valve a safeno-femoral reflux is developed and the blood column from the deep veins effuses to the superficial veins. This is how the pressure of the blood column is transferred through the superficial venous system towards the feet leading to vein enlargement.
Diagnostics
Besides the examination with a vascular surgeon or angiologist, when the anatomic position of the enlarged veins and the presence of inflammatory changes or clogs in the superficial veins is determined, the basic examination (especially before making the decision to do the surgical procedure or not) is an ultrasound (Doppler) of the leg veins. With it we determine the porosity of the deep venous system, the level of valve insufficiency and the flow of the superficial veins. A deep and superficial vein Doppler is an examination that must be done before any leg vein procedure.
Treatment
In the first stage of enlarged veins the operation treatment can be postponed by the usage od elastic-compressive bandages or stockings. Enlarged veins that have a diameter less than 2-4 mm can be treated with sclerosation. That is a method of injecting a solution of a sclerosing agent into the enlarged vein. Such and larger veins are also suitable for surgical removal under local anesthetics (mini flebectomy). This method consists of applying a local anesthetic in the area of the enlarged vein, small incisions in the skin (2-3 mm) and removing the enlarged vein with the help of special hooks. A compressive stocking is put on post operatively.
Atraumatic stripping
In the case of insufficient sapheno-femoral or safeno-popliteral valve, one of the methods that is indicated is used to remove one or two big superficial leg veins, the saphena magna vein and the saphena parva vein. We use so called atraumatic stripping of the superficial leg veins in our clinic. This procedure is performed by an experienced surgical team led by a renowned vascular surgeon. Enlarged leg vein operation in this case consists of implementing a special sonde into the previously tied superficial vein through a small incision in the groin area and its removal just under the knee joint, also through a small incision. Through small (2-3 mm) separate incisions left over enlarged vein offsets are removed. Atraumatic vein stripping in our clinic is performed in local anesthesia under sedation, and the patient is discharged a few hours after the procedure for home care. After this type of anesthesia, the recovery is a lot faster and easier in comparison to general anesthesia. It also brings fewer risks. The procedure is entirely painless for the patient and lasts about an hour with the preparation.
Preparation for the procedure
Although operation of enlarged veins is a routine procedure for our surgical team, a professional approach demands of us to dedicate special attention to preoperative preparation of the patient. The first step is the examination and consultation with a vascular surgeon in our clinic, during which we set an indication for a surgical treatment of enlarged leg veins and an operation date, as well as all other details concerning the surgery. After the examination and consultation, before the procedure, it is necessary to make an ultrasound (Doppler) leg vein examination, which will determine the porosity of the deep venous system, the level of valve insufficiency and the flow of the superficial veins. It is also necessary to do certain blood tests before the procedure. Before any surgical procedure, especially before enlarged leg veins surgery, patients need to stop with the usage of pain killers and nonsteroidal anti-inflammatory drugs, containing acetylsalicylic acid like Aspirin, Andol or Acisal. This is a very important factor in a patient’s preparation for surgical procedure, as this way we prevent possible bleeding and hematoma during and after the procedure. Following this instruction makes the recovery quicker and more successful, and the result of the operation is improved.
Recovery and sick leave
The main advantage of atraumatic stripping in comparison to standard methods is the significantly shorter recovery period. Elastic bandages are to be worn for 10 days following the surgery and after that it is sufficient to wear firm, elastic stockings for a period of two weeks. The final result of this operation depends on the course of the operation, the experience of the vascular surgeon and his team, it also depends on conscientious and detailed postoperative monitoring and control. To be sure of that we insist on regular check ups and everyday contact with the patient for our patients’ safety, successful recovery and postoperative monitoring. Ten days following the surgery the stitches from the small (2-3 mm) incisions, through which the procedure was done, are removed. In their place are left minimal, almost unnoticeable scars. After atraumatic stripping the advised sick leave and absence from work is a lot shorter than after a standard method, and they last from ten days to two weeks. The patient needs to rest a couple of days following the surgery.
Useful instructions for our patients
The patient has to do blood tests and a Doppler leg vein ultrasound.
Hemorrhoids
The term hemorrhoids refers to a condition in which the veins around the anus or lower rectum are swollen and inflamed. Hemorrhoids may result from straining to move stool. Other contributing factors include pregnancy, aging, chronic constipation or diarrhea, and anal intercourse. Hemorrhoids are both inside and above the anus (internal) or under the skin around the anus (external). Hemorrhoids (piles) arise from congestion of internal and/or external venous plexuses around the anal canal.
What Are the Symptoms of Hemorrhoids?
Many anorectal problems, including fissures, fistulae, abscesses, or irritation and itching (pruritus ani), have similar symptoms and are incorrectly referred to as hemorrhoids. Hemorrhoids usually are not dangerous or life threatening. Rarely, a patient can have bleeding so severe, that severe anemia or death may occur. In some cases, hemorrhoidal symptoms simply go away within a few days. But in most cases, hemorrhoidal symptoms eventually return, often worse than they were before. Although many people have hemorrhoids, not all experience symptoms. The most common symptom of internal hemorrhoids is bright red blood covering the stool, on toilet paper, or in the toilet bowl. However, an internal hemorrhoid may protrude through the anus outside the body, becoming irritated and painful. This is known as a protruding hemorrhoid. Symptoms of external hemorrhoids may include painful swelling or a hard lump around the anus that results when a blood clot forms. This condition is known as a thrombosed external hemorrhoid. In addition, excessive straining, rubbing, or cleaning around the anus may cause irritation with bleeding and/or itching, which may produce a vicious cycle of symptoms. Draining mucus may also cause itching.
How Common Are Hemorrhoids?
Hemorrhoids are very common in both men and women. About half of the population have hemorrhoids by age 50. Hemorrhoids are also common among pregnant women. The pressure of the fetus in the abdomen, as well as hormonal changes, cause the hemorrhoidal vessels to enlarge. These vessels are also placed under severe pressure during childbirth. For most women, however, hemorrhoids caused by pregnancy are a temporary problem.
How Are Hemorrhoids Diagnosed?
A thorough evaluation and proper diagnosis by the doctor is important any time bleeding from the rectum or blood in the stool occurs. Bleeding may also be a symptom of other digestive diseases, including colorectal cancer. The doctor will examine the anus and rectum to look for swollen blood vessels that indicate hemorrhoids and will also perform a digital rectal exam with a gloved, lubricated finger to feel for abnormalities. Closer evaluation of the rectum for hemorrhoids requires an exam with an anoscope, a hollow, lighted tube useful for viewing internal hemorrhoids, or a proctoscope, useful for more completely examining the entire rectum. To rule out other causes of gastrointestinal bleeding, the doctor may examine the rectum and lower colon (sigmoid) with sigmoidoscopy or the entire colon with colonoscopy. Sigmoidoscopy and colonoscopy are diagnostic procedures that also involve the use of lighted, flexible tubes inserted through the rectum.
How Are Hemorrhoids Prevented?
The best way to prevent hemorrhoids is to keep stools soft so they pass easily, thus decreasing pressure, and to empty bowels without undue straining as soon as possible after the urge occurs. Exercise, including walking, and eating a high fiber diet, help reduce constipation and straining by producing stools that are softer and easier to pass.
Hernia
Umbilical hernias occur around the navel and are common in women during or after pregnancy. They are often referred to as “outies”. Ventral or abdominal hernias occur when the intestine pushes through a weakening in the abdominal wall. They are frequently referred to as incisional hernias because the bulge often occurs at the site of a previous surgical incision. A groin or inguinal hernia can occur on one or both sides of the groin or scrotum. An inguinal hernia may be unilateral, occurring on one side of the groin, or bilateral, occurring on both sides of the groin. The majority of hernias are in this area and are most common in men. A direct hernia can be referred to as a “wear and tear” hernia, as weak tissue here can be aggravated by straining or lifting over time. About 30% of inguinal hernias are direct. Your doctor won’t be able to identify which type of hernia you have until you are in surgery.
Ganglion Cysts
In the hand, a ganglion is a particular type of lump which shows up next to a joint or a tendon. Inside, it is like a balloon filled with a thick liquid. It may be soft or hard, may or may not be painful, and may get bigger or smaller on its own. It may also be referred to as a mucous cyst, a mucinous cyst or a synovial cyst. Normally, joints and tendons are lubricated by a special liquid which is sealed in a small compartment. Sometimes, because of arthritis, an injury, or just for no good reason, a leak occurs from the compartment. Now, the liquid is thick, like honey, and if the hole is small, it can be like having a pinhole in a tube of toothpaste – when you squeeze the tube, even though the hole is small and the toothpaste is thick, it will leak out – and once it is out, there is no way it can go back in on its own. It works almost like a one way valve, and fills up a little balloon next to the area of the leak. When we use our hands for normal activities, our joints squeeze and create a tremendous pressure in the lubricating compartment – this can pump up a balloon leak with so much pressure that it feels as hard as a bone. The lubricating liquid has special proteins dissolved in it which make it thick and also make it hard for the body to absorb it when it has leaked out. The body tries to absorb the liquid, but may only be able to draw out the water, making it even more thick. Usually, by the time the lump is big enough to see, the liquid has gotten to be as thick as jelly.
Common sites for ganglions are
The wrist – on the back (“dorsal wrist ganglion”), on the front (“volar wrist ganglion”), or sometimes on the thumb side. These come from one of the wrist joints, sometimes aggravated by a wrist sprain. The palm at the base of the finger (“flexor tendon sheath cyst”). These come from the tube which holds the finger tendons in place, and are often due to tendon irritation – tendinitis. The back of the end joint of the finger (“mucous cyst”), next to the base of the fingernail. These can cause a groove in the fingernail, or rarely can become infected and lead to a joint infection. These are usually due to some arthritis or bone spurs in the joint.